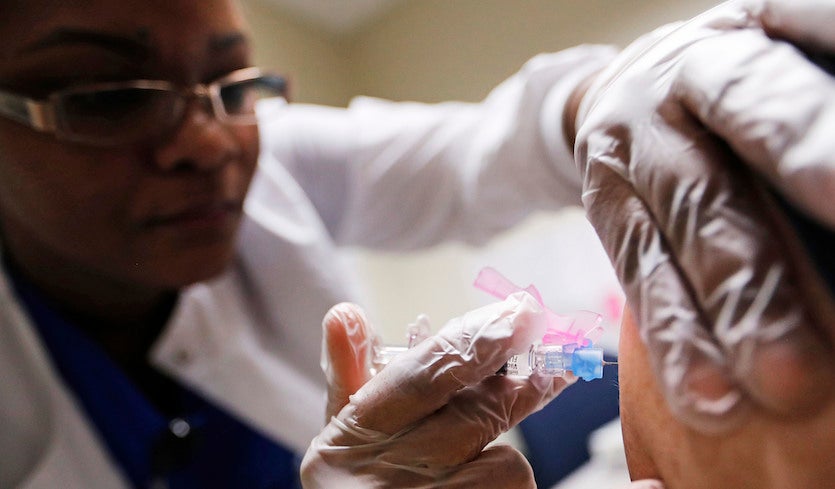
| Above: Registered nurse Claudina Prince administers a flu shot at a DeKalb County health center in Decatur, Ga., on Monday, Feb. 5, 2018. Image credit: AP Photo/David Goldman. |
Folk wisdom has it that cold weather predisposes you to a cold or flu bug. The truth is a bit more complicated—and a lot more interesting. Research over the past few years has zeroed in on atmospheric moisture as the main weather-related factor in flu transmission. The findings are especially relevant this winter, with the U.S. in the throes of one of its worst winters of flu in years, and its driest winter in more than three decades.
The key seems to be humidity levels inside, where people gather (and cough) during cold weather. Because it takes less moisture to saturate cold air than warm air, there can easily be high relative humidity (RH) outside on a bitterly cold day. However, once that air is heated to room temperature, the RH plummets.
Laboratory and epidemiological studies increasingly agree that the flu is transmitted more readily when the RH is low. At higher RH, the virus appears to be less stable, and the small virus-bearing droplets sent into the air by a cough seem more likely to attract water vapor and fall out of the air before infecting someone else. There’s also evidence that the flu grows more readily in the upper respiratory tract when it’s dry.
Experts agree that the atmosphere is not the main factor driving a flu outbreak. Instead, weather is more of a precondition that can leave the door open for flu to spread more easily. The moisture effect may not be large, but it’s robust and significant, according to Jeffrey Shaman (Columbia University), a leading researcher on the flu-weather connection.
 |
| Figure 1. Most of the U.S. saw below-average precipitation in December 2017, reflecting the dry air masses that predominated. The nationwide flu epidemic intensified dramatically from late December into January. Dry conditions remained widespread into January across many areas. Total precipitation for December-January across the contiguous U.S. (not shown) was the least since 1985-86. Shown above are statewide rankings for average precipitation during December 2017, as compared to each December since 1895. Darker shades of green indicate higher rankings for moisture, with 1 denoting the driest December on record and 124 the wettest. Image credit: NOAA/NCEI. |
 |
| Figure 2. Out of all outpatient visits to U.S. health providers, the percentage attributed to influenza-like illness (ILI) jumped from a baseline level of around 2% at the start of December 2017 (week 48) to nearly 6% by the end of the year (week 52). As of February 2, the percentage had climbed to 7.1%, approaching the peak of 7.7% that occurred in the 2009 pandemic. The hospitalization rate has now surpassed the peak from 2014-15, the most severe flu season of recent years. Image credit: U.S. Centers for Disease Control and Prevention. |
Why do we see more flu in the winter?
It’s taken a surprisingly long time to figure out how wintertime shapes the trajectory of flu outbreaks, said William Schaffner (Vanderbilt University), a past president of the National Foundation for Infectious Diseases. “Certainly the older explanation was always thought to be weak or insufficient—namely, when it gets cold, people go inside and they have more prolonged face-to-face contact,” Schaffner told me. “There’s probably some truth to that, but it doesn’t account for everything happening.”
Some of the first lab work pointing toward the moisture effect on flu was carried out a decade ago by Peter Palese, Anice Lowen, and colleagues at Mount Sinai School of Medicine. Using flu-infected and non-infected guinea pigs, a study led by Lowen found that relative humidities in the 20-35% range favored flu transmission from one animal to another, whereas no transmission occurred at an RH of 80%. Colder conditions led to greater transmission than warmer air.
A more recent study, published in PLoS ONE in 2013, looked at “artificial coughs” (produced by a nebulizer) in a lab setting held at a constant temperature, with the relative humidity varied across a range from 7% to 73%. Over an hour’s time, the influenza virus kept 71-77% of its infectivity when the RH was less than 24%, but only 15-22% when the RH was greater than 42%. “Maintaining indoor relative humidity >40% will significantly reduce the infectivity of aerosolized virus,” concluded the authors, led by John Noti (U.S. Centers for Disease Control and Prevention).
Building on this concept, Shaman and other researchers developed a mathematical model of flu transmission during outbreaks that takes humidity into account. In order to separate out the temperature and moisture effects, they turned to absolute humidity (AH, the amount of water vapor in the air). By doing so, they found in 2010 that AH far outweighed temperature as a determinant of flu spread in temperate (non-tropical) regions.
The findings were similar in a review of monthly flu-related mortality and weather patterns carried out for each of 359 urban U.S. counties from 1973 to 2002. Lead researcher Alan Barreca (now at the University of California, Los Angeles) found that absolute humidity of less than 6 g/kg was associated with greater mortality. This threshold corresponds to a sea-level dew point of around 43°F. If that outdoor air were brought inside and heated to a room temperature of 70°F, the relative humidity would be about 38%.
“Model predictions suggested that approximately half of the average seasonal differences in U.S. influenza mortality can be explained by seasonal differences in absolute humidity alone,” wrote Barreca and coauthor Jay Shimshack. “Temperature modestly influenced influenza mortality as well, although results were less robust.”
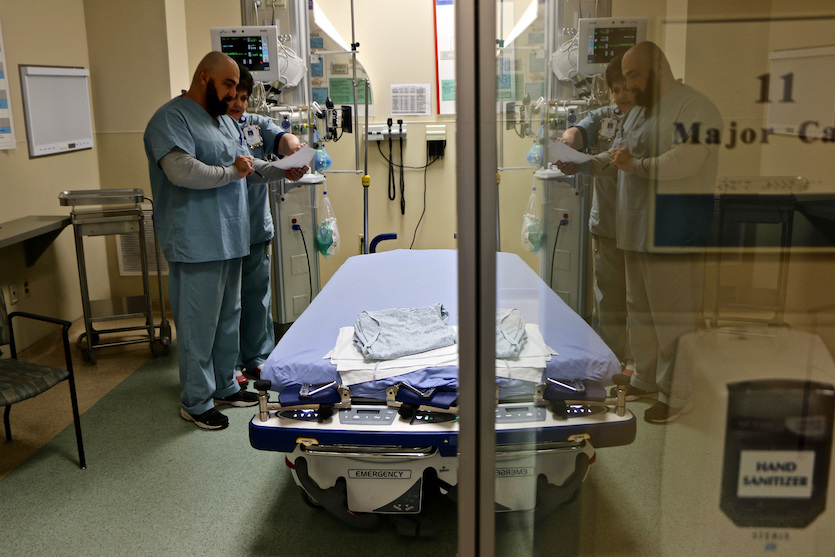 |
| Figure 3. A doctor and nurse confer inside a room used for flu patients at Northside Hospital in Cumming, Ga., near Atlanta, on Jan. 31, 2018. The U.S. government’s flu report released on Friday, Feb. 2, 2018, showed flu season continued to intensify in the previous week, with high volumes of flu-related patient traffic in 42 states, up from 39 the week before. Image credit: AP Photo/Robert Ray. |
Bringing the moisture effect into the forecast realm
Shaman’s latest work, published in 2017, finds that incorporating absolute humidity (AH) leads to a 3-5% improvement in forecast accuracy for models of flu transmission extending out to 4 weeks. Climatological values of AH helped even more than the values drawn from weather forecasts, perhaps because of the low skill in multi-week weather forecasts.
Even if the moisture effect on flu transmission is modest, it can still be useful. A team led by Dennis te Beest (Netherlands National Institute for Public Health and the Environment) found that absolute humidity explained about 3% of variation in week-to-week flu transmissions across the Netherlands from 1970 to 2013. “Although the influence of absolute humidity was small, its seasonal fluctuations may determine when sustained influenza transmission is possible and may thus drive influenza seasonality,” they noted.
In an email, Shaman used the analogy of hurricane development:
“In essence, climate/weather conditions provide the bounds, the envelope within which disease operates, much like hurricane activity is bounded by season, wind shear, sea surface temperatures, humidity, latitude, etc. However, that boundary forcing is not the dominant determinant of specific events, just as specific hurricane landfall events are not forecast solely based on broader environmental conditions. Infectious diseases, such as flu, have their own internal non-linear transmission dynamics that must be simulated to understand and forecast outbreaks.”
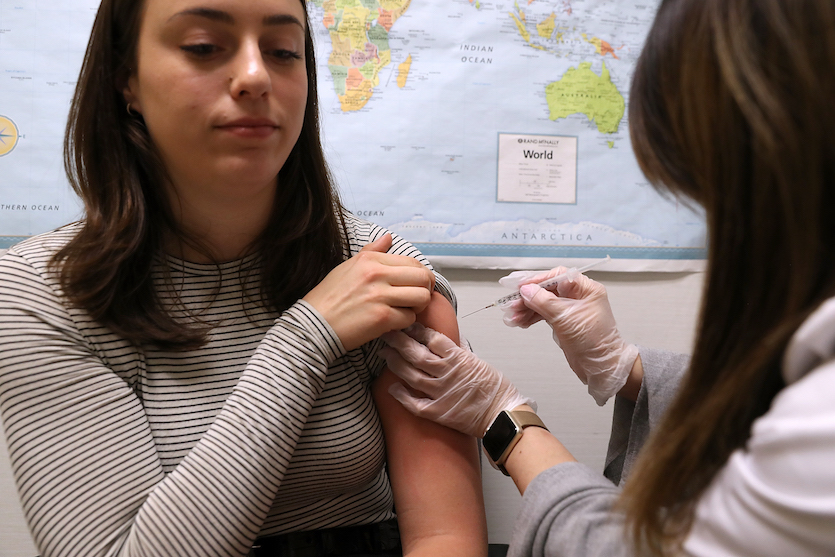 |
| Figure 4. Simone Groper receives a flu shot on January 22, 2018, in San Francisco, California. A strong strain of H3N2 influenza claimed the lives of 74 Californians under the age of 65 from October through mid-January. People are being encouraged to get flu shots even through the vaccine has been only 30% effective in combating the influenza. Image credit: Photo by Justin Sullivan/Getty Images. |
Climate change and the humidity effect
There could be a faint silver lining in climate change when it comes to flu and the United States. Absolute humidity is expected to increase in all seasons, with models indicating a 10-20% increase in wintertime AH over the U.S. by the end of this century, according to climate scientist Alicia Karspeck (co-founder of SK-Analytics), who’s collaborated with Shaman on previous work.
“At face value, this added environmental humidity would seem to act as a future protective factor against the flu,” Karspeck said in an email. “But due to the complexities of disease transmission, the opposite outcome has also been hypothesized—with earlier and more severe flu seasons becoming the norm. While there is little dispute that we are headed toward a warmer and more humid future, at this point there is still uncertainty as to how the seasonal flu will be impacted.”
 |
| Figure 5. A flu-stricken U.S. woman during the autumn of 1918. The Red Cross Home Service visited the woman, whose husband was in Europe as a World War I soldier. The global flu pandemic of 1918 killed an estimated 675,000 Americans, many of them in the space of just a few weeks. Image credit: U.S. Library of Congress, American National Red Cross photo collection. |
Time for a humidifier?
Last year, Alan Barreca moved from Tulane University, located in notoriously humid New Orleans, to UCLA, just in time to experience an unusually dry L.A. winter. Barreca’s home and office are both stocked with humidifiers, and he’s surprised that the health benefits of humidification get little notice.
“We don’t have the airtight evidence that a humidifier reduces your chance of getting sick, but we know that dryness is bad for you,” Barreca told me. Low relative humidity can dry out your nasal passages, making you more vulnerable to the flu virus and other bugs. Dehydration can also stress your cardiovascular system, noted Barreca. And there’s the greater likelihood that the flu virus will survive its trek from one person to another. Very high humidity can be a problem in itself, raising the risk of mold and other issues, but a midrange relative humidity of around 40% to 60% appears to be a sweet spot for overall health.
Boosting the humidity at your next Super Bowl party might not be a bad idea. Looking at years from 1974 to 2009, a recent study coauthored by Barreca in the American Journal of Health Economics found that metro areas with teams in the Super Bowl saw an average increase of 18 percent in flu mortality during that flu season among people age 65 and older. The increases were especially large when the game occurred closer to the peak of flu season and when the dominant flu strain was more lethal.
The authors speculate: “If the local population increases mixing as a result of team success, e.g., through private gatherings or attending sports bars to watch games, team success provides a proxy for shifts in socializing behavior during periods of traditionally higher influenza transmission.” Host cities—which presumably don’t have as many get-togethers as participant cities—didn’t see any significant increase in flu deaths.
The strains of flu that lead to the most severe global pandemics—such as the 1918 catastrophe that killed between 20 and 40 million, or up to one out of 50 people on Earth, many of them young adults—don’t need a boost from dry air. The worst phase of the 1918 epidemic peaked during September and October, not exactly what we think of as flu season.
“Virulence is outside of our control. It appears to be pretty random,” Barreca noted. “But humidity might be in our control, especially indoor humidity. That’s something we can do something about.”